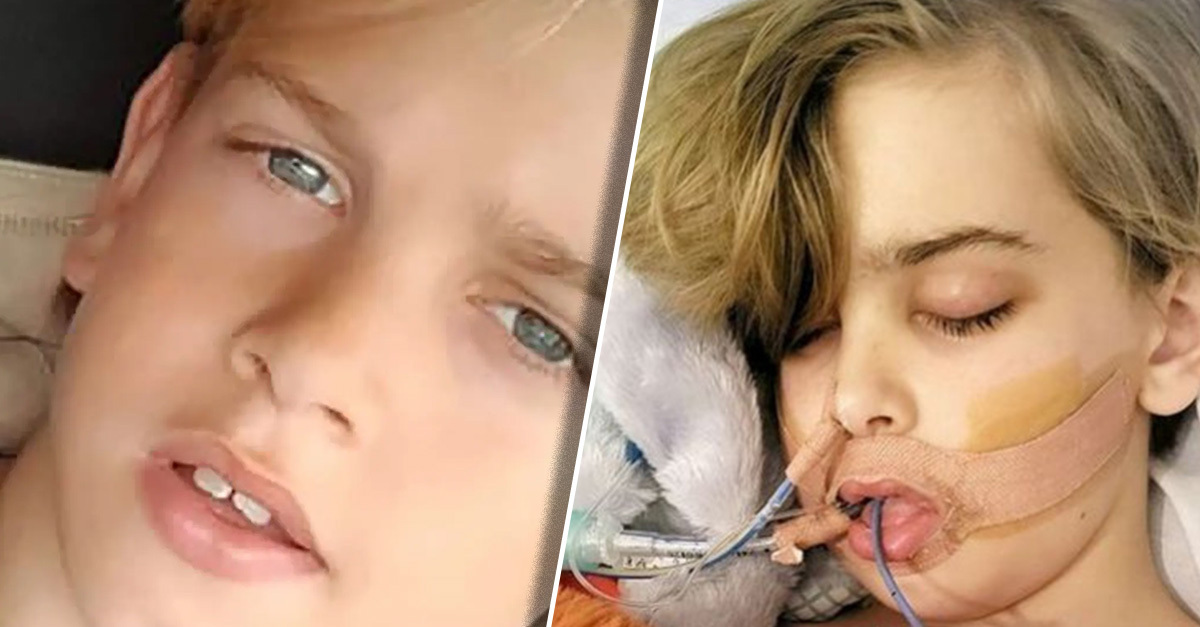
“My son has not been given enough time, and there have been miracles where people have come back from brain injuries…Until it’s God’s way, I won’t accept that he should go…He may not be the same as he was, but if there’s a possibility he could live a happy life after this, I want to give it to him.”
–Hollie Dance, mother of Archie Battersbee
As the pro-life movement celebrates the overturn of Roe v. Wade in the U.S. and the chance to save preborn children, another divisive issue is playing out in England on the other end of the pro-life spectrum: What is the value of a “damaged” or “deteriorating” human being, should that person’s life be terminated if there appears to be little hope, and — perhaps most controversially — who gets to decide?
These questions were front and center today when the U.K. Court of Appeal reviewed the case of Archie Battersbee, a 12-year-old with a brain injury who has been in a coma for three months. The court had agreed to decide whether to uphold or overturn a U.K. High Court order giving Royal London Hospital the legal permission it needs to turn off Archie’s mechanical ventilator, cease all medical treatments, and deny him any CPR or other lifesaving measures against his parents’ wishes.
Without appellate intervention, the ruling would have been a death sentence for Archie, who until April was a healthy, vibrant child who excelled in gymnastics and martial arts.
Fortunately, the three Court of Appeal judges quickly ruled that the evidence should be reconsidered by a different High Court to determine if it’s in Archie’s best interest for life-saving treatment to continue. Their decision means that the prior termination order is now on hold.
Archie’s parents, Hollie Dance and Paul Battersbee, have from the start refused to give up and have vowed to keep fighting for their child.
“My son has not been given enough time, and there have been miracles where people have come back from brain injuries,” said Hollie. “Until it’s God’s way, I won’t accept that he should go…He may not be the same as he was, but if there’s a possibility he could live a happy life after this, I want to give it to him.”
“A Troubling and Dark Precedent”
Archie came to be in his current condition after taking part in a dangerous online “blackout” dare in April that stopped his breathing for an estimated three minutes and left him in a coma. The hospital soon wanted to turn off his life support, but Archie’s parents, who are Christian (as is Archie), have refused to give consent, which is why the case went to court.
In the High Court’s decision on June 13, Justice Emma Arbuthnot ruled that Archie had technically “died” on May 31 based on MRI brain scans. She wrote,
“It is clear from the anxious and careful scrutiny of all the evidence including from clinicians with different specialties from five separate hospitals that tragically on the balance of probabilities, Archie is dead. I find that the burdens of treatment and his condition, along with the total lack of a prospect of recovery outweigh Archie’s Christian beliefs and the benefits of him continuing on mechanical ventilation for a few more weeks or months with all the other procedures that that entails.”
According to a statement from the Christian Legal Centre, which is representing Archie’s family, this ruling is “believed to be the first time that someone has been declared ‘likely’ dead based on an MRI test.”
Barrister Bruno Quintavalle, who argued on behalf of Archie’s parents, told the High Court that it was usurping Parliament’s authority by expanding the accepted legal definition of death in these types of cases. He explained:
“That the court should declare, in the absence of any certainty, that death has occurred is an extremely serious issue. If he is declared dead but actually isn’t dead, the consequences couldn’t be more grave.”
Andrea Williams, chief executive of the Christian Legal Centre, called the decision “devastating” not just for Archie and his family but for the future of a civil society. She stated:
“The idea that death can be declared on the balance of probability is frankly ludicrous. Life is the most precious gift that we have. This ruling sets a troubling and dark precedent. This case has raised significant moral, legal and medical questions as to when a person is dead. Archie’s parents do not accept that he is dead and are fighting courageously for his life.”
For her part, Hollie Dance, Archie’s mother, says she was “sickened” that neither the High Court judge nor the hospital took the family’s wishes into account and that the judge chose not to hear from independent medical experts who believe that Archie does, in fact, still have a chance at recovery.
Dance insists that Archie’s heart is still beating and that he has shown small signs of improvement, including having “squeezed my two fingers so tight they went bright red” and “only a few days ago, he began to open his eyes.”
She stated, “As his mother, I know he is still in there.”
Of Protocols and Miracles
Unfortunately, this is centralized, socialized medicine: a convoluted government-run bureaucracy where people — children, no less — are reduced to protocols, measures, numbers, resources, and the overarching goal of balancing the lives of individual patients with “the greater societal good.”
The family of Archie Battersbee is hardly the first to find their feelings, religious beliefs, and even the possibility of a second medical opinion and a chance to try elsewhere completely discounted within this cold, detached, pragmatic system.
In 2018, the U.K.’s National Health Service (NHS) turned off all life support for 23-month-old Alfie Evans over his family’s wishes. A court not only sentenced 11-month-old Charlie Gard to die over his parents’ objections but refused to allow them to take him home to die in familiarity, comfort, and love. The NHS even fought the parents of five-year-old Tafida Raqeeb when they asked for the opportunity to take her to Italy for treatment, insisting that taking her off of life support “was in her best interests.” Only after the case received international attention did a High Court allow them to do exactly that.
Tafida is now out of intensive care and continues to improve.
It’s not that NHS doctors don’t care; many of them often feel just as helpless and frustrated by the “tyranny of the rules” inherent in a government bureaucracy as do patients and their families. Physicians in such a system have been reduced to employee status rather than independent doctors, where their own unique experiences and medical judgments are disregarded and where they are required to practice according to treatment protocols and inflexible regulations.
The truth is that God alone has the “legal” authority to decide life and death, and He works miracles every day through medical professionals — even through those who don’t believe.
Last summer, Dr. Daniela J. Lamas, a pulmonary and critical care physician at Brigham and Women’s Hospital in Boston, experienced “a miracle” (her words) so unlikely and so overwhelming that she was moved to recount it in an article for the New York Times.
Her patient, a young father suffering from COVID-19 and a “cascade of complications, including pneumonia, sepsis, and devastating bleeding,” had been sedated and attached to a ventilator and lung bypass machine for more than a month.
“It was clear he was dying,” Dr. Lamas wrote, explaining that given “one medical catastrophe after another” the damage to his lungs had been rendered “not survivable.” She and her team told the family that it was time to give up and let go. His loved ones, devastated by the recommendation, asked for a few days to prepare to say goodbye before the machines were turned off.
But then the unexpected happened: That night, Lamas recalled, “my team watched in amazement as his oxygen levels started to rise, slowly at first and then steadily.”
The young father is now back at home with his family. “I marvel at the photographs they send me,” she says.
Dr. Lamas admits that she’s not always comfortable with the idea of “miracles,” but at the same time, she recognizes the possibility of the “one great save.” Certainly, popular medical biographies are filled with stories of sudden healings that no doctor can scientifically explain. In revisiting the patients “whose very survival proves us wrong,” she says, “I struggle with what to make of those outcomes and how to navigate the questions they raise.”
There is an explanation, of course, and it is nothing short of divine. The Bible tells us in 1 Thessalonians 3:17 to “pray without ceasing” and in Ephesians 6:18 to “pray in the Spirit on all occasions with all kinds of prayers and requests” — and that God’s perfect will always prevails, even in the face of impossible circumstances.
That is what parents do. They pray, they hope, they fight until they get a definitive answer. And sometimes God responds to a person’s faith and prayers and performs miracles. We see this in 1 Kings 17, wherein Elijah prayed and God raised the widow’s son from the dead, and in Mark 5:31-45, when Jesus Himself raised Jairus’ daughter from the dead, though some mourners scoffed at the possibility.
If God can raise a son or a daughter from the dead, He can heal Archie. There are simply too many stories of sudden “close to death, no chance of survival” turnarounds that can be attributed to nothing other than “God stepped in.”
“Until God Decides…”
Increasingly, of course, Western society has chosen to put its faith in medical technology and medical professionals, but neither is infallible — in fact, the No. 3 killer of Americans each year is related to medical error, according to a study by Johns Hopkins University.
What’s more, patients are routinely misdiagnosed — with doctors even getting death wrong. Take the case of Timesha Beauchamp, a 20-year-old woman with cerebral palsy who was declared dead, placed in a body bag, and transported to a funeral home. Imagine the surprise of a mortician to find that the corpse he was preparing to embalm was actually breathing! Timesha, it turned out, was still alive.
Archie Battersbee is still alive too, according to his parents and according to several independent medical sources. He has a beating heart. He responds to his mother’s voice. He can squeeze her hand.
And yet a single judge originally decided, based on different medical opinions and her own worldly sensibilities, that Archie is “dead.”
Of course, it’s possible Archie won’t survive but for a few more weeks and God will take him home. Or maybe he’ll awaken but get only slightly better, never again to be the same healthy, active, robust boy who once excelled in sports competition and made everyone laugh.
But by every moral and scientific measure, Archie Battersbee is still alive. What’s more, he is still God’s child and God has plans for his life.
His mother recently told a television interviewer, “…until God decides that it’s time for Archie to leave this world, I’m going to continue to be his voice and I’m going to continue to fight for his right to live.”
The courts and the hospital should respect the family’s wishes and leave room for God to make His plans for Archie fully known — but in His time, not the government’s.
Ready to dive deeper into the intersection of faith and policy? Head over to our Theology of Politics series page where we’ve published several long-form pieces that will help Christians navigate where their faith should direct them on political issues